
In one, little Joey Smelik is full of life and smiles, about to tuck into his third birthday cake.
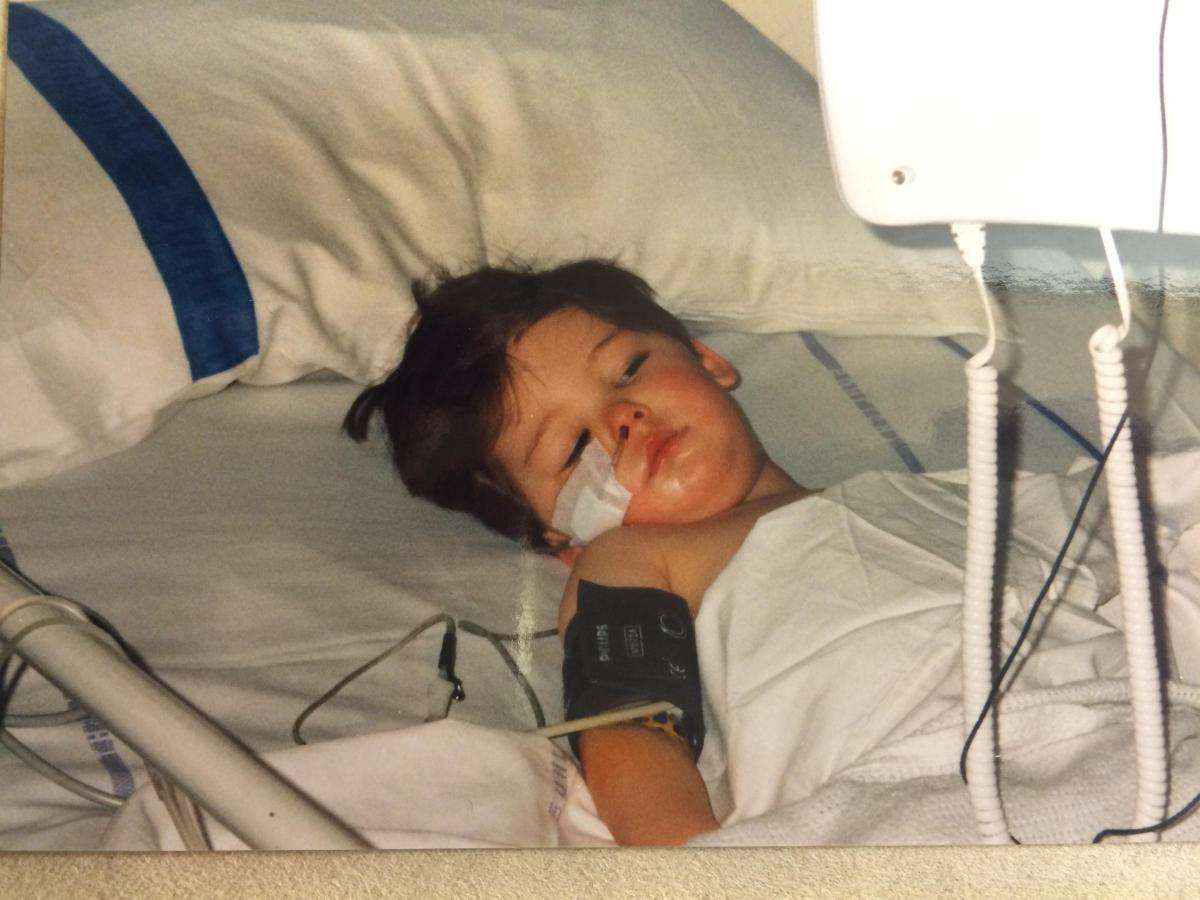
In the second, he looks a shadow of himself, in intensive care, following life-saving surgery.
The pictures were taken just three weeks apart - and are a painful reminder to his mother, Sarah, of how close she came to losing him.
Joey suddenly became ill one day while visiting his gran. Later that day, he couldn't stop vomiting. Sarah - an experienced mother with two elder sons - was not too worried, thinking it was a stomach bug. She visited the NHS out-of-hours centre and was reassured by a doctor it was probably nothing serious, but to call back later if concerned.
But the following day, Joey became worse. "He was still being sick and although he had been drinking water all day - gulping it down like he was desperately thirsty - his nappy was bone dry."
She telephoned the NHS out-of-hours service and explained the symptoms over the phone. She was asked if he had a temperature. Sarah felt his body; no, he wasn't hot. Was he alert? "Yes, he was alert," recalls Sarah, aged 48. "He was running around the house from pillar to post." When she inquired about the fact he had been drinking lots but had a dry nappy, she was reminded - rather patronisingly, she says - that young children can last for hours without going to the loo and that many were dry at night.
It was just enough to reassure her again, she says. However as the hours past, her gut instinct was telling her something was wrong.
"That night was one of the worst of my life," she says. "I didn't know what was wrong with my child. He was really ill all night, being sick and bringing up what looked like coffee grains, which I know now was dried blood. I tried to settle him and change his nappy but as I lay him down a noise came out of him like something I had never heard come out of a human. He was in serious pain. I was in a state of panic and worried. I didn't call 999, which I know now I should have done."
It wasn't until the following morning that Sarah saw another out-of-hours doctor, who told her to take Joey to hospital immediately.
As doctors examined him, they removed his nappy. Sarah says: "It was full of blood. That's when I realised it was serious."
An ambulance whisked Joey straight to a specialist paediatric surgeon in Leeds. The next few hours were a blur. "I got in the ambulance and the blue lights were going, " recalls Sarah. "I was sitting in the front and could see all the cars parting for us. I realised this was bad and went into shock myself."
In the operating theatre, surgeons discovered part of Joey's bowel had been cut off by an obstruction - a piece of sinew had wrapped itself around the bowel, acting like an elastic band, and pulled it tight, cutting it off. "All the bowel behind that had died and needed cutting out," says Sarah.

Sarah and Joey in hospital in Leeds
As Joey recovered in intensive care, Sarah learned the frightening symptoms he had displayed were of septic shock - an advanced and life-threatening stage of sepsis, where the body’s immune system goes into overdrive to fight infection but attacks its own tissues, risking organ failure.
Sepsis has been in the news in recent days following an apology by health secretary Jeremy Hunt to the parents of 12-month-old Cornish boy William Mead, who died in December 2014, after GPs, out-of-hours services and a 111 call handler failed to spot he had sepsis caused by an underlying chest infection and pneumonia. Mr Hunt said William was let down in the "worst possible way". A report into William's death has made recommendations relating to the 111 service that should be "treated as a national and not a local issue", concluded the politician.
He said: "(111) advisers are trained not to deviate from their script, but the report says they need to be trained to appreciate when there is a need to probe further, how to recognise a complex call and when to call in clinical advice earlier.
"It also highlights limited sensitivity in the algorithms used by call handlers in the signs relating to sepsis."
Sarah couldn't agree more, but believes opportunities were missed from Joey's case which happened 11 years ago, to improve call handlers' and medics' awareness of sepsis and its complications such as septic shock.

Sarah and Joey today, and on the right, Joey's scar
Joey made a good recovery and is about to turn 14. He wears his abdominal scar like a badge of honour, but for his mum, it reminds her of the her darkest hours when she nearly lost him.
Afterwards, she wrote to doctors in an effort to make sure no-one slipped through the net like Joey.
On reflection, she believes if the call handler had asked different questions, Joey might have been diagnosed with a life-threatening condition sooner.
Instead of asking if he had a temperature, the question should have been: 'What is his temperature?' A low body temperature can be a sign of sepsis and septic shock.
Instead of asking if he was alert, the question should have been: 'Is he agitated?' This can be a another indicator.
A third warning sign was missed too - that Joey had been drinking lots of water but not urinating.
Sarah hopes Joey's story will raise awareness - every year in the UK there are 150,000 cases of sepsis, resulting in around 44,000 deaths.
She said: "Please learn the signs, and if your gut tells you something is wrong, please follow it."
Sepsis fact file
1 Sepsis is a life threatening condition that arises when the body’s response to an infection injures its own tissues and organs. Sepsis leads to shock, multiple organ failure and death especially if not recognized early and treated promptly.
2 Only one in three people with severe sepsis or septic shock get the basic treatment that could save their life within the safe timescale of one hour.
3 Every year in the UK there are 150,000 cases of sepsis, resulting in a staggering 44,000 deaths – more than bowel, breast and colon cancer combined.
4 It can affect all ages and can follow from something as apparently harmless as a scratch or flu. It’s also relatively common after childbirth or surgery.
5 Every hour that it goes untreated raises the risk of death by eight per cent. One in five of those who do survive are left with long-term damage to organs such as the kidneys, lungs and the liver.
Find out more at: sepsistrust.org





Comments: Our rules
We want our comments to be a lively and valuable part of our community - a place where readers can debate and engage with the most important local issues. The ability to comment on our stories is a privilege, not a right, however, and that privilege may be withdrawn if it is abused or misused.
Please report any comments that break our rules.
Read the rules here